“Mama gena neve, mage duwa gena salakilimath venna.”
It’s not about me, take care of my daughter, was the plea of the mother as she drifted off to unconsciousness induced by anaesthesia.
This was no ordinary mother-daughter duo – they are the pioneers who have put Sri Lanka well and truly on the transplant map. For they are the first donor-recipient pair of a 24-hour “living donor liver transplantation” that a trailblazing team of doctors from the Kelaniya Medical Faculty performed without much fanfare at the Nawaloka Hospital in Colombo on October 15.
 |
| Mother and daughter: Now all smiles |
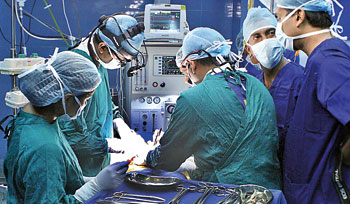 |
| The transplantation underway |
Both mother, U.K.G. Muthu Menike, and daughter, Niroshani Kumari Thoragolla, from Nawalapitiya are well on the road to recovery. Last week, Menike, 51, had left for home while Niroshani, 26, had been discharged from hospital and was hoping to move into an annexe close to the Ragama Teaching Hospital to be reviewed by the doctors for about six weeks.
When the Sunday Times met some of the young and excited doctors on Tuesday, they underscored the fact that the first successful living donor liver transplant ever to be performed in Sri Lanka owes its outcome to perfect team work. The team of about 50 not only doctors but also nursing and other support staff worked in tandem, they said.
The operation with military-like precision began at 7.30 a.m. on Saturday, October 15, with Menike being wheeled into the operating theatre first. A battery of tests had been carried out before, soon after mother and daughter decided without hesitation, that they would like to proceed with the transplant after both the positives and negatives had been clearly explained to them by the doctors.
The “matching” process included not only the blood group but also the body size and the size of the liver, explains Consultant Surgeon, Dr. Ruwan Wijesuriya who headed the surgical team. While this Transplant Surgeon managed the recipient and guided the full team, his Co-Transplant Surgeon, Dr. Rohan Siriwardane headed the team focusing on the donor.
“The body size correlates to the liver,” points out Hepatologist Dr. Madunil Niriella, citing the example of a small liver not being suitable for transplant in a large person. The mother’s “liver health” had also been screened through a biopsy and imaging because the donor’s safety was of paramount importance.
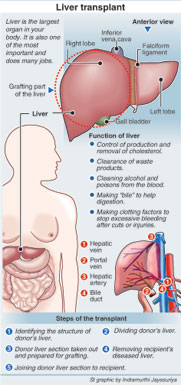
The largest organ in the body, the liver may be compared to the vital engine of a car. It contains billions of specialized cells that are linked to a well-organized system of bile ducts and blood vessels which form the biliary system.
The liver is also unique because it has the amazing ability to regenerate or create new liver tissue.
The match was perfect, says Dr. Niriella, while the donor-mother was healthy.
As part of the donor’s liver, 60%, was being harvested (see graphic for details), the Surgeons were not tense, assures Dr. Wijesuriya, for, they had often done resections (removal of parts) of diseased livers at Ragama. However, a “technically demanding aspect” is the extrication of the liver from all its connections, as it is joined to many parts of the body.
The drugs are costly |
Please give a helping hand to
Niroshani Kumari Thoragolla who needs to take costly immuno-suppressants lifelong by contributing your mite to her account 053200180010982 at the Nawalapitiya
People’s Bank. |
The other “crucial moment” is the time the harvested liver section “has to be on ice”, points out Consultant Surgeon Dr. Chandika Liyanage, explaining that this has to be minimal. To achieve this, the recipient should have been opened up and the diseased liver extricated by that time.
It was around 8 p.m. that it was done and the team smiles when asked whether tiredness did not creep on them because they had been on their feet for 12 hours. “We are used to long operating hours,” is Dr. Wijesuriya’s simple reply.
What of food during the long haul?
After about four to five hours we did have a nibble, a sandwich or a roll, they say, while Dr. Liyanage quips, “We didn’t eat rice though.”
It was less than an hour that the donor liver section was on ice, the Sunday Times learns. Removing the diseased liver of the daughter, the next task was gently lowering the mother’s resected liver into the cavity and linking it to key structures of the body including the hepatic vein, the portal vein, the hepatic artery and the bile duct.
The team also had to be alert for haemorrhaging, as “blood loss” could spell disaster. “There was minimal blood loss,” says Dr. Wijesuriya.
Blood loss is the “dread of the anaesthetists”, stresses Consultant Anaesthetist Dr. Bhagya Gunetilleke, for even though the donor is perfectly healthy, torrential blood loss would create a crisis on the operating table. In the case of the recipient the blood vessels are abnormal due to the disease and hypothermia is what they need to look out for.
“Our job is to keep the patient alive, anaesthetized maintaining stable blood pressure, ventilated and pain-free. The surgeons need the patients to be adequately relaxed for easy accessibility to the organ,” he says shuddering at the “riskiest situation” when the moment the new liver is re-perfused (supplied with fluid), the patient bleeds, the blood pressure drops and the potassium levels go up causing an abnormal heart rhythm.
The Surgeons would like us to reduce the central venous pressure as bleeding is less and we do that while maintaining the blood flow to the other vital organs. We also keep the patient warm to prevent hypothermia setting in, says Dr. Gunetilleke, creating the image of the tightrope that anaesthetists walk.
By 11 p.m. that Saturday, Menike was in the Intensive Care Unit while daughter Niroshani followed only at 6.30 a.m. the next day, when finally the weary team put down their scalpels and scrubbed down.
Sunday was victory day, for the mother was off the ventilator by noon and the daughter at 6 p.m. Day 7 after the transplant, the mother is discharged and the daughter two weeks later.
A heavy regimen of immuno-suppressants, as many as 10 a day, is administered to the daughter as the chances of rejection are highest during the first three months after the operation.
Multiple drugs are given during this time to stop her body from rejecting this “foreign” organ even though the matching has been spot on, explains Dr. Niriella, with the medication being tapered down after that. She will, however, be on immuno-suppressants life-long, it is learnt.
“Amma will go back to tending the small tea land that we have along with Apochchi,” says Niroshani, chirpy and bright, when the Sunday Times contacts her on the phone.
For Niroshani whose fiancé has been by her side like all her relatives through this experience, marriage is on the cards, “maybe in a year”, while in about six months she will seek a job in the field of her choice, environmental science.
Struck down by Wilson’s disease
Niroshani suffering from Wilson’s disease had been referred to the Ragama Hospital as it had the biggest liver disease programme since 1995. Three years ago hepatobiliary services had also been included under the same roof.
Physicians, surgeons and anaesthetists are working together as an organized team, said Consultant Hepatologist Dr. Madunil Niriella, explaining that Ragama had become the national referral centre for chronic liver disease. However, till surgeons joined up it was providing only supportive treatment to prolong and temporarily improve the quality of life of the patients.The only hope for these patients being a liver transplant, some struggled to find the money to get it done abroad, while others died, the Sunday Times understands. It was to India that most went spending as much as Rs. 8 million each.
By this time Ragama was handling the most number of liver resections, after having self-innovated and self-funded the programme as there was a lack of equipment, says Surgeon Dr. Chandika Liyanage.
They could, however, see the urgent need for liver transplants and the team launched into harvesting livers from cadavers. But the wait for a cadaver was long and so far they have been able to do only two such transplants, in May and July, this year.Patients were perishing, at least one or two a month or just falling off the wait-list, lamented Surgeon Dr. Ruwan Wijesuriya.
The only option was living donor transplants and that’s what they have done in the case of Niroshani who had end-stage liver disease or cirrhosis due to excessive copper in her body which had damaged her liver. Niroshani’s family, like thousands of middle-class families, just could not afford to take her abroad for this life-saving treatment.
Determined to carry out the transplant, the team faced the next major hurdle – Ragama Hospital did not have the essential equipment for this major surgery such as the Cavitron Ultrasonic Surgical Aspirator (CUSA), blood-gas machines, near-patient coagulation monitors, rapid blood infusers et al. But the doctors knew of a hospital which did have them – Nawaloka. CUSA is needed to resect the liver and reduce intra-op blood loss.
When approached, Nawaloka willingly agreed to support them, and absolutely free of charge, in memory of the hospital’s founder H.K. Dharmadasa and his wife, while the team of doctors also waived their full fee.
The team comprised Consultant Surgeons Dr. Ruwan Wijesuriya, Dr. Rohan Siriwardane, Dr. Chandika Liyanage, Dr. Sumudu Kumarage, Prof. Aloka Pathirane and Dr. Harsha Gamage; Consultant Anaesthetists Dr. Bhagya Gunetilleke, Dr. Nilmini Wijesuriya, Dr. Sagarika Ranasinghe and Dr. Asantha de Silva; Registrars Dr. Rasitha Wijewantha, Dr. Senita de Silva, Dr. Ayesha Maduwanthi and Dr. Chinthake Appuhamy; Medical Officers Dr. J.K. Mithinda, Dr. Hasika Nagahawatte, Dr. Dushyanthi Jayasekera, Dr. Lasantha Jinadasa, Dr. Dinesh Weerasinghe and Dr. Senerath Bandara; Consultant Hepatologists Prof. Janaka de Silva, Dr. Anuradha Dassanayake, Dr. Madunil Niriella, Prof. Arjuna de Silva and Dr. Mettananda Nawaratne; Consultant Pathologist Prof. Janaki Hewavisenthi; and Consultant Radiologist Dr. Sanjeewa Munasinghe supported by the Ragama Hospital nursing staff headed by Staff Nurse Sandaseeli as well as Nawaloka Hospital’s theatre, ICU and liver unit staff headed by K.T. Fernando and Sister Hettiarachchi.
The transplant would not have become a reality without the unstinting cooperation of Ragama Hospital Director Dr. Roy Perera and Nawaloka Chairman Jayantha Dharmadasa and General Manager/Director Prof. Lal Chandrasena, is the consensus among those involved in this “first” for Sri Lanka. |