Is the "cure" equally bad or worse than the bite? Rushed to the nearest hospital after being bitten by a deadly sarpaya, are the hopes and expectations of men, women and children that they would be saved from death unfounded?
Groundbreaking and striking research for the successful treatment of snakebite by making anti-venom safer by reducing the risk of severe allergies has been done right here in Sri Lanka, bringing this tiny island to the fore. (See box)
Adrenaline, the treatment |
The “treatment” for the anti-venom side-effects which the medical teams administered to snakebite victims from the sealed envelopes consisted of adrenaline, promethazine and hydrocortisone, and placebos, alone or in different combinations.
Injecting a small dose of the inexpensive and widely available adrenaline under the skin just before administering the anti-venom is safe and effective in significantly reducing the risk of acute severe allergic reactions, the research has found.
Promethazine made no difference while hydrocortisone by itself also made no difference. However the adrenaline-hydrocortisone given in combination counteracted or aborted the positive effects of adrenaline, the Sunday Times understands. Meanwhile, most reactions to the anti-venom occur immediately after it is administered or within the first hour, it has been found.
There is no more need for trial and error when treating snakebite with anti-venom – one treatment that has been ascertained is – the humble adrenaline neutralizes the adverse side-effects of anti-venom. When treating snakebite with anti-venom -- adrenaline saves lives.
|
Crisscrossing the country at least once a month during three long years, from March 2005 to April 2008, the meticulous, time-consuming and tiring but finally rewarding research was conducted at five different sites by Principal Researcher Prof. Asita de Silva and his team from the Clinical Trials Unit of the Kelaniya Faculty of Medicine at Ragama. The research was carried out in the North Central Province, the North Western Province, the Sabaragamuwa Province and the Southern Province well-known for large numbers of snakebites.
Undertaken in collaboration with the University of Oxford and the Liverpool School of Tropical Medicine, the research was funded by small grants from the University of Kelaniya and the University of Oxford and supplemented by funds provided by the reserchers themselves.
For the "partners" on the ground, the dedicated and diligent members of the medical and nursing teams headed by Consultant Physicians at Anuradhapura (Dr Shaluka Jayamanne), Polonnaruwa (Dr Ariyasena Hittharage), Kurunegala (Dr Ranjith Kalupahana), Embilipitiya (Dr Asoka Ratnatilake) and Hambantota (Dr Senarath Samarakone) Hospitals who with great care and precision followed the protocols laid down by the research team, it was of public interest. Long days and long nights were the lot of the three sets of research coordinators at each site, chosen from doctors who had passed out of the Kelaniya Medical Faculty and were awaiting internship postings, whose duty it was to scrupulously record all trial-related details in "pre-prepared" clinical record forms.
Christmas, New Year, poya or any other holiday, they worked because snakes don't have holidays, jokes Prof. de Silva, explaining that the stream of snakebite victims flowed into the hospitals day and night, 24/7.
In keeping with international protocols including strict adherence to norms and guidelines with regard to patients, with clearance being obtained not only from the Health Ministry but also the Ethics Review Committee of the Faculty of Medicine, University of Kelaniya, the researchers set to work, screening each and every patient who came to the five hospitals after snakebite.
They screened over 4,600 patients, anyone over 12 years of age with a "history" of snakebite. "In a clinical trial it is important to screen consecutive patients to avoid choosing only patients who fit our preconceived notions," says Prof. de Silva.
From this huge number, more than 1,000 patients were randomly distributed to different treatment options in this clinical trial which is perhaps the largest snakebite trial undertaken in the world, he says.
Explaining the need for such a study, Prof. de Silva says that when a patient is brought to hospital after being bitten by a venomous snake, the victim is administered the anti-venom after careful clinical examination and monitoring when systemic envenoming is diagnosed. However, the polyvalent (given for the bites of five types of snakes) anti-venom imported from India, though effective, causes side-effects in the form of allergies in the snakebite victim, ranging from mild to moderate to severe.
The deadly snakes in Sri Lanka, of the many snakes here are: Russell's Viper or Daboia russelii russelii (Sinhala -- thith polonga or dhara polonga; Tamil - kanardi viriyan), Cobra or Naja naja (Sinhala - nagaya or naya; Tamil - naga pambu or nalla pambu), Common Krait or Bungarus caeruleus (Sinhala - thel karawala or maga maruwa; Tamil - yennai panayan, yennai viriyan or yettadi viriyan), Sri Lankan Krait or Bungarus ceylonicus (Sinhala - dunu karawala or polon karawala; Tamil - yennai panayan, yennai viriyan or yettadi viriyan), Saw-scaled Viper or Echis carinatus (Sinhala - veli polonga; Tamil - surattai pambu or pal surattai), Hump-nosed Viper or Hypnale hypnale (Sinhala - polontelissa; Tamil - kopi viriyan) and the sea snake. Ninety percent of envenoming and deaths are caused by the Russell's Viper, the Cobra and the Common Krait.
The use of poor quality anti-venom manufactured in India is fraught with danger. Weak effiectiveness could mean that huge volumes of anti-venom need to be given to the victim, leading to acute danger of serious allergic reactions including anaphylaxis. When 10 to 20 vials are pumped into patients, the treatment can be even more dangerous than the initial snakebite. The quality of the anti-venom that is currently available here is poor and impurities such as equine proteins found in it cause the allergies in humans, points out Prof. de Silva.
The allergies could be just a mild rash or severe anaphylaxis, stresses research team member, Dr. Channa Ranasinha, giving the repercussions of the anti-venom in numbers. "A huge 75% of those administered the anti-venom develop allergies and for 40% these allergies are life-threatening. The allergies could include an itchy rash, faintness and becoming unconscious, swelling including of the throat, wheezing, vomiting, cramping stomach pain and diarrhoea. Some may go into shock due to these and die," he adds.
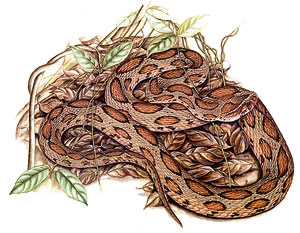 |
| One of the deadly snakes: The Russell's Viper or Daboia russelii russelii . Pix courtesy of ‘Snakes of Sri Lanka-- A coloured atlas’ by Anslem de Silva with illustration by Jayantha Jinasena |
Doctors have been grappling with this problem of the cure being equally bad or worse than the bite for decades in the peripheral health units of Sri Lanka and research to improve safety of such anti-venom preparations has been ongoing here as well as across the world but the evidence has been inconclusive.
Groping in the dark without concrete answers, doctors have been administering antihistamines and hydrocortisone alone or in combination, before giving the anti-venom to prevent these allergies which inexorably affect 75%. Will it work, has always been a fear nagging them as they watch their snakebite patients and hope for the best.
This is what the research team was determined to find out. Until the quality of the polyvalent anti-venom is improved, which too is crucial, the mission of the researchers was to find out which antihistamine or combination acted best in preventing the allergies triggered by the anti-venom.
When asked why they undertook this research, Prof. de Silva says the main reasons were snakebite being a major public health problem and the urgent need to find a local solution to improve safety of anti-venom by reducing acute reactions to it. In Sri Lanka, more than 35,000 patients are admitted to hospitals annually after snakebites and about 1, 200 die an agonizing death. A research team from the same Medical Faculty led by Prof. Janaka de Silva estimated the global burden of snakebite for the first time and published the results also in PLoS (Public Library of Science) Medicine in 2008. This groundbreaking work resulted in the World Health Organization classifying snakebite as a 'neglected tropical disease'.
The paperwork was immense and the planning meticulous. It was at the Clinical Trials Unit of the Kelaniya Faculty of Medicine that the important envelopes not only with the study medications - adrenaline, promethazine and hydrocortisone -- but also placebos (a matching substance but containing no medication) in different combinations were placed and the sealed envelopes sent to the five hospitals for use in snakebite treatment.
The medical teams at the hospitals did not know what they were administering because it was a "blinded" clinical trial and the code was known only by two persons at Ragama who too were available 24/7 for the three years. For they had to respond if there was a crisis with a snakebite victim and a need to break the code and tell the doctors what they had been administering. "The patients' safety was of paramount importance," says Prof. de Silva.
As soon as the medication was given before the anti-venom, the "close monitoring" began, with the coordinators recording various clinical features including blood pressure, heart rate, level of consciousness and peak respiratory flow rate, at very regular intervals (every 15 minutes during the first two hours) for the next 96 hours.
After every 200 patients, an international data safety monitoring committee was given "unblinded data" from the study to ensure patient safety. All trial centres were audited or checked by the Liverpool School of Tropical Medicine on two occasions during the study period to ensure data quality and adherence to protocol. If the international data monitoring team felt the patients in the trial were in any danger or it was unethical to continue if some treatment was showing clear evidence of efficacy or adverse effects, the clinical trial would have been suspended, says Prof. de Silva.
By April 2008, there were more than 4,600 data sets to be analysed, a gargantuan task handled by Prof. Arunasalam Pathmeswaran, a statistics expert of the Kelaniya Medical Faculty. Once completed, the research team was on the home-run writing up the paper and submitting it to the prestigious online medical journal, Public Library of Science (PLoS) Medicine in March 2010.
Stringent reviews by six diverse peers spread from Australia to Bolivia followed with comments such as "defining study" and research that will "revisit snakebite history".
Vindication of the hard work came when in May this year PLoS Medicine published the research team's findings not just as a research paper but as the "Editor's Choice" itself.
|


