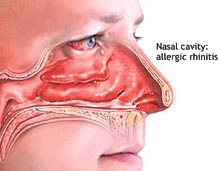
There are many of us who start the day with repeated bouts of sneezing, runny nose and itchy eyes. Despite the discomfort some of us would have lived with this for so long, we might even consider it normal. Allergic rhinitis as this condition is known, is not normal but it is not a sinister problem either and can effectively be controlled with medication.
This week Dr. Melanie Amarasooriya speaks to Dr. Bandula Bandaranayake, Consultant ENT Surgeon at General (Teaching) Hospital Kegalle about allergic rhinitis.
Allergic rhinitis is common: Even though in Sri Lanka statistics are not available, in the west it is said to affect every one in five people. It is commoner in children - in 80% of patients the condition would have started before the age of 20 years. However, this could affect anyone, at any age. Children do tend to outgrow this problem. It tends to run in families, being commoner among children whose parents have had the condition.
Allergic rhinitis is characterized by the inflammation of the nasal mucosa, the delicate lining of the nasal passage, due to allergy. With time this inflammation can affect the lining of the throat, the sinuses, middle ear and the eyes. For some people the allergic response is to dust, for some it’s animal dander or pollen. In the majority they are allergic to a variety of substances and commonly a single allergen is not easy to identify.
Symptoms
When the nasal mucosa is inflamed you feel the irritation of the nose, repeated sneezing and runny nose. You might feel that nasal secretions are dripping down from the back of the nose to the throat --- ‘post nasal drip’. Your eyes will be itchy and red. In addition you will feel irritation of the throat, stuffy or congested nose and fullness in the ears. With time, this can bring about dark circles on the skin around the eyes.
This troublesome condition, is quite similar to a common cold. For people with allergic rhinitis it is as if they are having a cold every day, in some people there is a seasonal variation, which is not quite commonly observed in our country.
“It’s a clinical diagnosis, investigations are not routinely done to diagnose allergic rhinitis,” says Dr. Bandaranayake. “However complete examination of the patient is mandatory as it could be associated with other conditions like sinusitis or nasal polyps.” Nasal polyps are harmless mucosal swellings from the delicate internal lining of the nose. Though they are not harmful they will add to the discomfort of nasal block.
Treatment
“Treatment of allergic rhinitis is all about effectively controlling the symptoms so that the patient’s everyday activities are not disturbed. There are several options,” says Dr. Bandaranayake, stressing that the mainstay of treatment is the steroid spray.
One simple treatment modality is to avoid any identified allergens. For instance, people who are allergic to animal dander may benefit from keeping away from pets. However, avoiding allergens is not quite practicable as people are usually sensitive to several substances and it is difficult to individually identify them. Therefore, it is not strictly advised to give up everything that you enjoy; Medication can be a help to control the disease instead. These drugs are designed to reduce or combat the allergic response.
The most prescribed treatment for allergic rhinitis is the steroid nasal spray. When it comes to using steroids people are reluctant to use them. There is also this common stigma about inhalers in asthma and sprays in allergic rhinitis.
Steroid sprays are nothing to be alarmed about. They simply prevent inflammation occurring at the site. Steroids do have side-effects as do all other medications. But these are common when steroid tablets or injections are taken for a long time. Sprays exert their effects at the site with less absorption of the drug to the body. Hence the side effects are minimized by administering the drug directly to the site of the problem in this case to the nose.
The condition in nasal mucosa in allergic rhinitis is quite similar to what happens in the lungs and air passages in asthma. In fact in the patients with generalized allergic tendency these two conditions can co-exist.
The other medication is tablets of antihistamine category. These drugs tend to cause sleepiness. But there are newer drugs without sedating effects. However these are not sold over the counter in our country.
It’s important that you do not self treat this illness, for several reasons. One is there are other problems that may mimic allergic rhinitis or there could be co-existing problems that need extra attention. Also, when complications of this disease occur such as chronic sinusitis, the antihistamine and spray are inadequate. You will need antibiotics and sometimes drainage of collected secretions under local anaesthesia.
Your friends’ pill will not suit you even if have the symptoms seem to quite similar. As patients with allergic rhinitis repeatedly complain of nasal block, the chances are that they may be self-prescribing nasal decongestants repeatedly. This can worsen the condition due to rebound enlargement of the nasal mucosa. Therefore patients are advised not to use nasal drops more than the duration in the prescription. Over the counter use of nasal decongestants is not advisable. However, they can be good symptom relievers when used short term, 3 to 5 days.
Nasal sprays: How to use them correctly
Nasal sprays are different from inhalers used for asthma, even though the active ingredient in the drug may be similar. The composition of medication and the container is different to deliver the drug with maximum effect to the relevant site. Therefore do not mistake your inhaler with the spray though the name may sound similar.
Nasal sprays come in two different kinds of containers: pressurized canisters and pump bottles.
First, blow your nose lightly to clear the secretions before using the spray.
Shake the bottle or the canister well.
Do not blow the nose or sneeze just after using the spray.
Use your medicines the way your doctor tells you. Most nasal sprays work best when used regularly and consistently.
Keep your medicine away from sunlight.
When using the canister;
Slowly breathe out, while keeping your head upright.
Close one nostril with your finger and with the other hand hold your spray to the other nostril.
Press down the canister, and start breathing through that nostril at the same time, while keeping the other nostril closed.
Do the same to the other nostril and repeat if necessary according to the number of puffs you are recommended.
When using the pump bottle;
You may need to prime the bottle by squirting a few times into air until a fine mist comes out, when it's used for the first time on a day.
Breathe out slowly as you tilt your head slightly forwards.
Hold the pump bottle with your thumb at the bottom and your index and middle fingers on top.
Use a finger on your other hand to close your nostril on the side not receiving the medication.
Breathe in as you squeeze the pump. Repeat to the other nostril and as prescribed. |