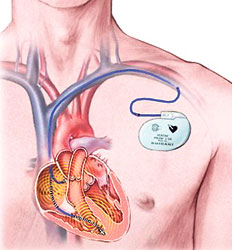
A pacemaker is used when the heart cannot beat regularly and when there is an abnormal rhythm which persists. This little device prompts the heart to beat on time. Your cardiologist would decide whether you need a pacemaker depending on your condition.
There are different types of pacemakers and your cardiologist will decide which type is best suited to you. You will have to undergo an operation (usually under local anaesthesia) to get the pace maker inserted under the skin of your chest.
Benefits of a
pacemaker:
A pace maker does not cure your heart disease. But it keeps your heart pumping regularly for years by sending electric pulses to the heart. Hence it improves the quality of your life. You will have relief from symptoms like faintishness and dizziness which you may have been experiencing. You may feel more energetic and can lead a normal full life with it.
What are the risks?
Complications due to the operation, such as infection, blood loss
In rare cases, the device can be displaced. Then the effect of the pacemaker can be defective.
After coming home
from surgery:
Keep the wound clean and dry. Contact your doctor if it seems infected.
Use only gentle movements with the arm closest to the pacemaker. Avoid stretching, lifting and sudden jerky movements. Gradually increase the use of your arm.
Carry your pacemaker identification card with you at all times
As each person’s recovery period is different, ask your doctor when you can return to work, drive and exercise.
You can indulge in leisure activities once you have recovered, though you should avoid rough contact sports like rugby, football or strenuous exercise.
Contact your doctor if;
You feel tired, short of breath or if you start experiencing the symptoms you suffered from previously like feeling faint.
The wound gets infected - feels red, hot, swollen, painful and starts oozing
Importance of
clinic visits
You need regular follow-up clinic visits as instructed. At each clinic visit, the performance of your pacemaker is checked by placing electrodes. Talk to your doctor about any discomforts or worries you may have.
Usually the battery of a pacemaker lasts 5 – 10 years. It takes several months over a period of several months to run down. At each follow-up visit your doctor will check the battery and once the period is over, another pacemaker will be inserted by means of another operation.
Remember…..
Certain electrical and magnetic energies can interfere with your pacemaker.
When coming into contact with medical equipment – MRI scanning, cancer radiation therapy etc – always inform that you have a pacemaker
Metal detectors and security systems used in airports - When you enter or leave a place with a security system, walk through the entrance / exit at a normal pace. Do not stay long near those areas.
Home electrical appliances in good working order can be used safely, eg microwave ovens, blenders, toasters, televisions, VCR, stoves etc)
X Rays, CT scans, US Scans and mammography are safe
Inform the doctor when you go for any medical or dental procedure, that you are on a pace maker.
You can use a mobile phone without any problem but do check with your doctor to make sure. Activated mobile phones should not be kept in your shirt pocket.
Conditions which cause muscle twitching and shaking movements can inhibit your pace maker. These include Parkinson’s disease, vigorous rigors in malaria, urine infection, fits etc. Inform your doctor if you develop such a condition.
Rhythm of the heart
Your heart has its own internal electrical system that controls the rate and rhythm of your heartbeat. With each heartbeat, an electrical signal spreads from the top of your heart to the bottom. As the signal travels, it causes the heart to contract and pump blood.
Each electrical signal normally begins in a group of cells called the sinus node or sinoatrial (SA) node. As the signal spreads from the top of the heart to the bottom, it coordinates the timing of heart cell activity.
First, the heart’s two upper chambers, the atria, contract. This contraction pumps blood into the heart’s two lower chambers, the ventricles. The ventricles then contract and pump blood to the rest of the body. The combined contraction of the atria and ventricles is a heartbeat (Courtesy MedicineNet.com).
(The writer is attached to the Health Education Bureau) |