News
NHSL: Meeting the challenge of raging COVID-19
- No patient will be turned away, whether COVID or non-COVID, assures Deputy Director-General Dr. Kumara Wickremasinghe
- Premier institute now the largest COVID treatment hospital in country
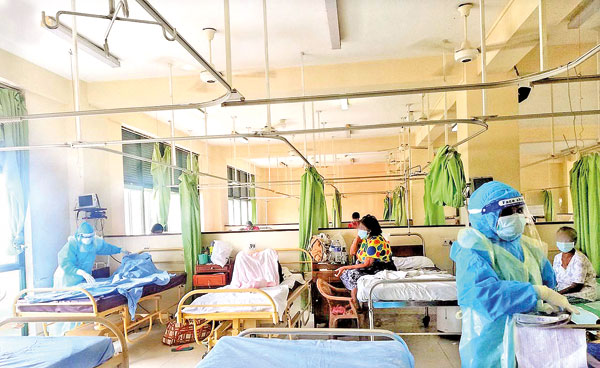
Recovering from COVID-19 in a comfortable bed with staff in attendance at the NHSL
A busy day as usual – patients walking in and out of the premier National Hospital of Sri Lanka (NHSL) in Colombo and the staff going about their work, as siren-screaming and red-light flashing ambulances turn in through its gates.
Within this sprawling hospital complex, there has been a major change and it is to discuss this matter of crucial importance to the people of the country that the Sunday Times is here on Friday.
“The NHSL will never turn away any patient whether COVID or non-COVID,” is the reassuring message from the Deputy Director-General (DDG) of the NHSL, Dr. Kumara Wickremasinghe who is at the helm, guiding its massive operations through consultation with his staff.
In these desperate times of COVID-19 with numerous people pleading for a hospital bed, the Sunday Times has experience that he is speaking the truth.

Dr. Kumara Wickremasinghe
When contacted in the past weeks, senior NHSL doctors have advised COVID-19 positive patients or those with COVID-19 like symptoms to come to Gate 5, to be triaged at the Fever Corner and then be directed either for admission, to an intermediate care centre (ICC) or for home-based care.
After having two minor tosses, an 80-year-old had consulted his Cardiologist at a private hospital. When he tested COVID-19 positive, he had been advised to go to the NHSL.
This is what he did and now he is receiving treatment at the NHSL.
When initially the pandemic hit the world early last year, the NHSL was not a designated COVID-19 Treatment Centre. As the COVID numbers were not that large in the first and second waves, the 3,250-bed NHSL played the role of a screening centre, for its catchment area of patients is huge. Not wanting to jeopardise all those who sought medical or surgical succour, the staff initially carried out RT-PCR tests and subsequently Rapid Antigen Tests and isolated those affected by the virus, acting as a comfortable holding centre until they could be transferred to a COVID Treatment Centre.
“We commissioned a medical and surgical ward to accommodate these COVID-19 patients and attended to their medical needs until the transfer took place,” explains Dr. Wickremasinghe.
With the third wave engulfing the country and the COVID-19 Treatment Centres being overwhelmed by an influx of patients, the time had come for the NHSL to step-up its role and do what it does best – meet the needs of the people without compromising its care.
The DDG says that more and more wards were mobilized for the care of COVID-19 patients with major efforts being made to provide a comfortable in-ward bed for each and every one.
“This was done in consultation and with the support of the full-range of staff. We took into account the changing needs, especially the oxygen-dependency of positive patients who were coming in,” says Dr. Wickremasinghe, reiterating that they continue to perform other emergency and life-saving surgeries and medical procedures in all specialities.
They are also not neglecting other patients including those who come in with heart attacks, stroke, kidney failure and dengue, while patients attending regular clinics can call for advice and come in if something is worrying them. The medications of clinic patients are sent by post to them.
Before COVID-19 struck, the NHSL usually got around 1,000 Outpatient Department (OPD) visits and had about 750 admissions daily, while performing on average 5,000 surgeries per month.
Dr. Wickremasinghe says the NHSL’s journey has been successful and evolving with the strong support of the Health Ministry, the security forces and donors who came forward…….with equipment, consumables or to renovate or convert sections to have negative pressure in an ICU setting to prevent the virus from spreading.
The donations have amounted to Rs. 90 million (Rs. 50m worth of medical equipment, Rs. 10m worth of non-medical equipment, Rs. 10m worth of consumables and ward renovations to facilitate wall oxygen amounting to Rs. 20m).
“The NHSL has adequate storage facilities for oxygen with a large tank of 20,000 litres being on site. So far, the daily patient requirement of oxygen is about 10 tons. We have made the access to the tank easier so that filling it up can be done conveniently,” says Dr. Wickremasinghe, an example of how each detail has been looked into.
Referring to human resources, he says the challenge is to prevent healthcare staff from getting infected so that they can provide maximum care to the patients. They are provided Personal Protective Equipment and those working in COVID-19 wards are from a pool so that there is weekly rotation which helps in not taxing one group only.
Even though the NHSL did not conduct RT-PCR tests initially, now it has a fully-equipped laboratory to do so, with RAT being initiated in November last year and RT-PCR testing in January this year, with the capacity of 200 RT-PCRs in two cycles in 24 hours.
Looking into all the key aspects of running such a marathon operation including human resources, infrastructure upgrades and facility improvements, the NHSL’s secret in evolving into the largest COVID-19 Treatment Centre in the country lies in meticulous planning, while looking ahead and foreseeing the needs of people.
So far, the NHSL has treated 10,600 COVID patients and lost about 400, says Dr. Wickremasinghe with a tinge of sadness, adding that in the last two weeks the number of positive patients receiving their care sometimes went up to 665 per day.
He fervently appeals to people to get themselves vaccinated as a majority of those who have died are the elderly, mostly unvaccinated, and those with co-morbidities.
“Vaccination prevents severe disease and death,” he underscores.
The NHSL with its dynamic staff of 8,000 has risen to meet a national emergency with 18 wards dedicated for COVID-19 treatment.
With the number of beds edging close to 700 (697 to be exact) including 217 beds with oxygen delivery and 100 High Dependency Unit beds, what the DDG says rings not only loud and clear but also true.
“We will not turn away any patient,” a message of hope for the hapless victims of COVID-19.
| A new 100-bed ICC The NHSL has opened and is managing on its own a 100-bed Intermediate Care Centre (ICC) just a stone’s throw from the main hospital, next to the Cardiology Institute since Monday. “In a laudable gesture, the Salvation Army gave this building to us when the country is facing this crisis and we converted it into an ICC with the help of the Health Ministry,” says Dr. Kumara Wickremasinghe. Both male and female patients can be accommodated here. This is while the NHSL is also tending to 100 more beds along with other stakeholders at an ICC in Rajagiriya. Appreciating the home-based care system launched by the Health Ministry for asymptomatic (without symptoms) and mildly-symptomatic patients, Dr. Wickremasinghe says that it has helped to relieve the load on hospitals. Stressing the need to reduce the infection numbers, he appeals to all people to take the health precautions (face-mask wearing, hand hygiene, keeping more than a 1.5 metre distance from others in public places and not leaving home unless it is absolutely essential) and safeguard not only themselves but also their loved ones. | |
| Don’t let the air leak in from the sides of the face maskWith myths about face-masks doing the rounds, many experts underscored that a face-mask is essential to keep the virus at bay. Echoing the views of many others, one expert said that no intervention is 100% effective. But face masks can reduce infection if they are used properly. Face-masks are one of the essential health measures including washing hands or using sanitizer frequently when out of home, keeping at least a 1.5 metre distance from others in public places and avoiding crowded places and closed spaces. “The face mask should be worn properly. It should securely cover the nose and mouth and not be allowed to slip down. There should also be no gap, even a small one, between the face-mask and the cheeks,” he said, adding that the mask should rest securely on the cheeks. If there is a gap, it could lead to an air-leak into the nose and mouth which are being protected from the virus. |

