Sunday Times 2
Lanka as diving medicine hub
One was on holiday here and the other was in the Maldives with the second part of her tour bringing her to Sri Lanka.

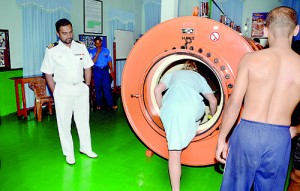
Physics of pressure: Surgeon Rear Admiral of the Navy Dr. Lalith Ekanayake says diving medicine can promote tourism. Left: A patient entering the Recompression Chamber at the Trinco Naval Base. Pic by Nilan Maligaspe
The 30-year-old Sri Lankan now domiciled in England was in Hikkaduwa and the 30-year-old New Zealander was in the Maldives when they were both hit by lethargy and numbness just last month.
There was only one common factor – both had been diving before these symptoms surfaced. A search on the web and they found that Sri Lanka had the only Consultant in Diving Medicine in the whole of Southeast Asia, while the ‘Recompression Chamber’ that was needed to help them recover fully was available at the Trincomalee Naval Base.
“Many people don’t realise the dangers associated with diving and give scant regard to the essential measures that need to be adhered to,” points out Diving and Hyperbaric Medicine Consultant Dr. Lalith Ekanayake, who is Surgeon Rear Admiral of the Navy.
Before jumping into diving physiology and diving medicine, he is quick to point out the need for Sri Lanka to promote this rare expertise and facility within the Navy.
Urging that a ‘Recompression Chamber’ should also be set up in Colombo to treat victims of diving illnesses, Dr. Ekanayake suggests Welisara as “ideal”.
 With Sri Lanka promoting tourism and the sun, sea and sand being major attractions, diving medicine should play an important role, according to him and he has already initiated discussions with the Peradeniya Medical Faculty to incorporate such a segment in its curriculum.
With Sri Lanka promoting tourism and the sun, sea and sand being major attractions, diving medicine should play an important role, according to him and he has already initiated discussions with the Peradeniya Medical Faculty to incorporate such a segment in its curriculum.
Smilingly explaining that humans are not fish and we perform breathing essential for life in one atmosphere, he creates an image of what happens when a person dives deep under water which is a “risky environment”.
Usually when breathing, we take in 21% of oxygen and 79% of nitrogen but as we go under water, the atmospheric pressure increases gradually. The deeper you dive, the atmospheric pressure becomes more. While the diver is breathing air which he has collected at the surface, as he goes deep down, he begins to breathe under pressure, he says.
In the deep, nitrogen, an inert gas, which has been inhaled becomes a liquid and circulates with the blood of the diver. Oxygen which 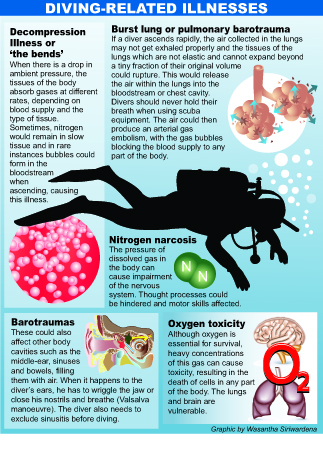 acts the same way is however active. “As long as you are in the deep it’s okay. Trouble hits the diver when surfacing, as the reverse doesn’t happen at the same speed,” says Dr. Ekanayake, adding that nitrogen under pressure turns into bubbles increasing in volume. When the diver is surfacing, the volume doubles in the last 10 metres.
acts the same way is however active. “As long as you are in the deep it’s okay. Trouble hits the diver when surfacing, as the reverse doesn’t happen at the same speed,” says Dr. Ekanayake, adding that nitrogen under pressure turns into bubbles increasing in volume. When the diver is surfacing, the volume doubles in the last 10 metres.
What should happen is that the nitrogen should come to the lungs and be exhaled. This is why every diver has to plan his dives taking into account the depth of the dive, how much time he will spend at the seabed and what should be the time duration between dives, the Sunday Times learns.
The modus operandi before dives should be to feed these data into a computer and get a diving plan, which would clearly indicate the surfacing strategy which may sometimes include a stop of at least half an hour at 10 metres.
When the diver surfaces, the decompression due to the pressure stops and if the nitrogen bubbles in the blood don’t go out of the system, they get into the circulatory system and could create an embolism, in this case a gas bubble, says 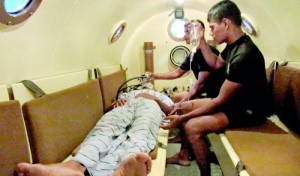 Dr. Ekanayake.
Dr. Ekanayake.
In the wake of such a scenario could come severe illness, he points out for if the embolism enters the brain, there could be a stroke; in the heart, there could be a heart attack; in the spinal cord, there could be paralysis; in the joints, there could be aches and pains; and in the skin there could be numbness.
Any diver who has numbness, confusion, joint aches and pains, urinary problems, undue fatigue, chest pain, unsteady gait, fever or loss of memory within 48 hours of a dive, should immediately suspect that these symptoms are linked to diving, stresses Dr. Ekanayake.
The person in Hikkaduwa who had done multiple dives to 30-34 metres, experienced weakness on the left side and numbness in various parts of the body.
It was ‘Decompression Illness’ or ‘The Bends’, says Dr. Ekanayake.
Looking for help, his family had come across the information about Dr. Ekanayake on the web and contacted him. Having examined him in Colombo, with the permission of Navy Commander Vice Admiral Jayanath Colombage, he had him transported to Trincomalee.
Three sessions of treatment in the ‘Recompression Chamber’ administered by Surgeon Commodore Easajith Jayasinghe and Surgeon Lieutenant Commander Chandana Attanayake at the Trincomalee Naval Hospital under the guidance of Dr. Ekanayake had made the symptoms disappear.

Under the watch of Navy doctors, Navy divers undergoing treatment inside Recompression Chamber
“He was 100% okay,” says Dr. Ekanayake, explaining that the New Zealander, meanwhile, came to him in a more roundabout manner. Having done a couple of dives in the Maldives, she had experienced weakness and lethargy and also developed an unsteady gait. Feeling slightly better after being administered oxygen over there, she had flown to Sri Lanka which was next on her holiday itinerary.
What she didn’t realise was that her recovery was only temporary, he says. In Sri Lanka, she did what was not appropriate following a diving illness. She went up to Nuwara Eliya which is at a high altitude and later climbed the Dambulla rock. Exertion and travelling at high altitudes are a definitive “no, no” after a diving illness.
When diagnosed, the patient should be made to lie flat and given plenty of fluids, either orally or intravenously as there has been loss of hydration and also volume depletion. When being transported for treatment, the patient should be taken at sea-level or if flown it should be at a low altitude, it is learnt.
Not adhering to any of this, the New Zealander had gone about her holiday but panic gripped her when the numbness in her body worsened. Surfing the net, she too had come across the Diver Alert Network (DAN) which pointed her in the direction of this Consultant in Diving Medicine.
“Usually for decompression illness, the patient should be treated within 48 hours,” underscores Dr. Ekanayake, but she came in fairly late. However, the New Zealander received three sessions of treatment in the chamber, recovered 100% and flew back home, he says, adding that the decision to send a patient into the ‘Recompression Chamber’ should be taken after a risk-benefit assessment.
For, the ‘Recompression Chamber’ could be claustrophobic, the environment strange, the treatment lengthy ranging from 45 minutes to 4-5 hours. The patient’s mobility is also restricted.
| Dalton, Henry, Boyle and Charles: Physics of diving
Diving related illnesses could be caused during irregular ascent and descent, as well as at the bottom of the sea. This is due to divers having to breathe a gas which is at the same pressure — called ambient pressure — as their surroundings, which can be greater than on the surface, explains Dr. Ekanayake, adding that several laws in physics come into play. They include Dalton’s Law (solubility and diffusion of oxygen and nitrogen in our body depend on the partial pressure); Henry’s Law (the volume of a gas that can be dissolved in a liquid is directly related to the partial pressure of the gas to which the liquid is exposed); Boyle’s Law (the pressure of a gas decreases as the volume of a gas increases); and Charles’ Law (if pressure and the amount of gas remain constant, the volume of the gas increases or decreases by the same factor as its temperature). Some of the main disorders that could be caused by breathing gas at the high pressure encountered at depth are decompression illness which includes decompression sickness and arterial gas embolism; nitrogen narcosis; oxygen toxicity and pulmonary barotrauma or burst lung. (See graphic) |

