Wracked by a persistent cough for more than three weeks? Don’t be frightened but at the same time don’t ignore it. Get yourself tested for tuberculosis (TB).
For, early diagnosis of TB is of vital importance, stresses the Director of the National Programme for TB Control and Chest Diseases (NPTCCD), Dr. Sunil De Alwis, explaining the disease which sees as many as 9,000 new cases in Sri Lanka every year.
With early diagnosis and treatment of the diseased person, the spread of the infection can be curbed while the quicker the treatment starts the better the outcome for the person who is already ill, he says. “As respiratory infections spread quickly in the community, each person who is found positive for TB during sputum tests, if not treated quickly can infect 10-15 new healthy people every year.”
What is TB?
It is an infectious disease caused by Mycobacterium tuberculosis. There are two other types of Myco bacteria, causing TB, but are not so common in Sri Lanka. TB mainly affects the lungs (80%). Other organs which can fall victim to this bacterium include the brain, bones, spine, lymph nodes, eye and skin etc (20%) . TB can affect any tissue or organ of the body.
Seeing the way TB consumes the patient’s body from within, in the past it has been called "consumption" and in indigenous medicine “kshya rogaya”.
Symptoms
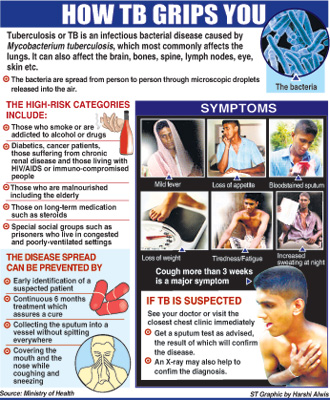
These include a cough for more than three weeks, mild fever and sweating particularly in the evenings, loss of appetite, loss of weight, tiredness and fatigue, with bloodstained sputum as a later symptom. Sputum is defined as matter coughed up and usually ejected from the mouth, including saliva, foreign material and substances such as mucus or phlegm, from the respiratory tract.
“If TB is suspected, see your doctor immediately or visit the closest chest clinic,” advises Dr. De Alwis, explaining that a sputum test or an X-ray of the chest will confirm whether it is TB.
Dispelling the misconception that TB is a hereditary disease passed through the genes from parent to child, he stresses that it is an air-borne infectious disease spread from one infected person to others
who are healthy.
In the lungs Myco bacteria multiply and cause extensive tissue damage only when the host’s body conditions are favourable. A battle erupts between the body’s immune system and the bacteria, as the bacteria attempt to spread to other parts. Detailing the process, Dr. De Alwis explains that the immune system forms scar tissue or fibrosis around the TB bacteria to prevent their spread throughout the body. If the body's immune system is unable to fight them and they break through the scar tissue, the infection turns into the diseased status.
 |
Unlike in other infectious diseases the “infection” and “diseased” are two different clinical entities -- not all infected persons become diseased. It is estimated that one third of the population in the world are already infected with TB leading to 8 million new diseased people and 2 million deaths per year. Thirty-five percent of the global case-load is in the South Asia region and 20% of the global disease burden in India alone, according to the World Health Organization (WHO). In Sri Lanka, the level of infection is around 40%, says Dr. De Alwis.
From the public health point of view, of all TB patients, the sputum positive ones (those who produce sputum containing bacteria) are the most dangerous. Some patients with lung TB, however, do not produce bacteria-containing sputum and such are not infective to others. Therefore sputum examination is not only a reliable diagnostic tool, but also important to design and plan preventive measures.
In Sri Lanka, there are about 5,000 sputum-positive cases per year. Unfortunately, some people are reluctant to get their sputum examined, which is freely available, explains Dr. De Alwis, adding that the referrals from medical officers for sputum microscopy in both public and private sector, other than in the chest clinics are extremely low. “It is the cheapest, most cost effective and reliable diagnostic tool for TB in the world recommended by the WHO and it is a pity that most sputum microscopy centres are highly underutilized,” he laments.
It is noteworthy that 25% of TB patients get cured “themselves” even without medical intervention due to regained immunity advancement. Better nutrition and improved, well-ventilated and sunny environments will empower the immune system over the bacteria. Nevertheless 25% of patients die within five years and the others live a little longer with chronic illness, while infecting others. The patients who are on treatment are not infective to others after two weeks of such treatment, Dr. De Alwis stresses.
Therefore, TB in a person can be categorized as either “latent” or “active”. Latent TB occurs when the bacteria are present but inactive and there are no symptoms. It is not contagious. However, active TB in which a person manifests symptoms makes that person ill as well as being contagious.
How does TB spread?
When someone with active TB coughs, sneezes or even laughs, he/she expels the bacteria into the air as droplets and when a healthy person breathes or inhales them, they enter the lungs causing the TB infection.
“About half of those who inhale the bacteria are able to destroy them through their strong immune systems, while about 40% will have latent TB and become diseased only if their immunity goes down. Only 10% of those infected will get the disease because their immunity is low at the time,” says Dr. De Alwis.
Is there a vaccine?
The BCG vaccine available for TB usually protects children and infants from the severe childhood forms of the disease, but adults can contract it even after being vaccinated as children. All children in Sri Lanka get the BCG soon after birth which has caused a dramatic reduction of TB among children. If a child below 5 years does not have a ‘BCG scar’ on his/her left upper arm, the BCG should be given again.
It is better to prevent TB by eating a healthy diet to boost your immunity, says Dr. De Alwis, assuring, however, that even if you get TB it can be cured. “It is essential to take the right medication in the correct dosage at the correct time for the period prescribed which is usually six months. The Direct Observation Treatment (DOT) short course has been introduced under which an observer watches while the patient swallows the medicine.”
The number of tablets has also been reduced. With the introduction of the fixed dose combination, fewer tablets have to be taken, he says, adding that many people stop taking their medication when they feel better.
Don’t do that, urges Dr. De Alwis, stressing that the whole course of drugs is vital to rid the body of TB. “If you stop the medications halfway, the bacteria will multiply to such an extent that normal medication will not be able to deal with the disease, causing multi-drug resistant TB.”
Defaulting is a serious problem in Sri Lanka. Usually patients stop the treatment or take the medicine in an irregular manner. This may be due to negligence from the patient or his relatives, but in most of the cases it is also due to a false sense of feeling better, as after a few weeks of treatment most of the symptoms disappear. But the consequences of stopping the medication is disastrous, as the disease will be there, may be in a worse form that is difficult to cure.
While complicating matters and having to take more expensive drugs for a longer duration, such TB could also result in death, he warns.
Health services
- Chest clinics in each district where treatment can be sought without a referral from a doctor
- Microscopic centres in peripheral hospitals in all districts to conduct sputum tests
- DOT at heath facilities and also community based
- In partnership with the private sector, drugs will be issued to private practitioners free of charge if the patient wants to continue his treatment with his practitioner.
- Screening of contacts, both at workplace and in the household
- Tracing of defaulters if the patient does not come in for treatment.
Awareness programmes aimed at early detection
Dealing with the disease situation in Sri Lanka, Dr. De Alwis says that the WHO country estimate for each year for new patients infected with TB is 11,000 but the TB Programme has been able to identify on average about 9,000 each year.
Pointing out that either the country estimate is not accurate or there is a gap in case detection, the Director says that a concerted effort has been launched to sensitize medical officers, general practitioners, politicians, the media and the community on the need for early detection. A colourful calendar hanging in his office is the result of an art competition held on TB among schoolchildren.
TB infections are vastly different in the urban-rural situations, MediScene learns with Colombo district including Colombo city having the largest number of new infections amounting to about 2,000 each year. The other vulnerable areas are the Gampaha and Kalutara districts.
The Programme is also focusing on the elderly, the estate population and prisoners, it is understood. The elderly not only in homes but even living with relatives could be vulnerable because they may be malnourished and when sick unable to seek treatment quickly due to financial and transport issues. “However, we need to be extra careful because in most homes very young children are looked after by the elderly and if infected with TB could easily pass it on to them,” he says. |


