Dyspepsia is a recurrent or persistent pain or discomfort that is primarily located in the upper abdomen. The "discomfort" is an uncomfortable feeling but does not reach the level of pain. It is mainly concentrated in the upper abdomen, although a person may also have pain in other areas. Approximately 25 percent of people worldwide experience dyspepsia.
 |
| Pix courtesy Getty images |
Dyspepsia can develop as a result of various underlying conditions . However, the most common type of dyspepsia is "functional" (or "non-ulcer") dyspepsia. This refers to dyspepsia that occurs without an identifiable cause.
Symptoms
People with dyspepsia can have one or more symptoms, including indigestion, discomfort or pain in the abdominal area, bloating, an early sense of fullness with meals (early satiety).
Some patients with dyspepsia also experience nausea, vomiting, a lack of appetite, weight loss, or other symptoms and findings.
Types of dyspepsia:
There are two major categories of dyspepsia: "Functional" dyspepsia refers to the dyspepsia that occurs with no obvious abnormality in the digestive tract. "Organic" or "non-functional" dyspepsia refers to conditions that have a visible abnormality in the digestive tract.
Causes
It is not clear what causes the signs and symptoms of functional dyspepsia. However, researchers have focused on several factors that may be involved.
Motor or nerve coordination - Normally, the process of digesting food involves a complex series of events that requires coordination of the nerves and muscles of the digestive tract. Abnormalities in this system may lead to delayed emptying of the stomach contents into the upper region of the small intestine, resulting in nausea and vomiting, an early sense of fullness with eating, and bloating. Delayed gastric emptying is found in approximately 30 percent of people with dyspepsia. However, many people with delayed gastric emptying have no symptoms of dyspepsia.
About 40 percent of people with dyspepsia have impaired relaxation (also called accommodation) of the upper region of the stomach after meals. This can cause an early sensation of fullness.
Visceral sensitivity - Enhanced visceral sensitivity is an increased sensitivity to pain, or a lower threshold for pain, that occurs when normal stretching or enlargement of the stomach occurs. Studies have consistently shown that people with functional dyspepsia often have visceral hypersensitivity.
Helicobacter pylori infection - Helicobacter pylori (H. pylori) is a bacterial infection of the stomach that can lead to inflammation (gastritis) or ulcers. There may be a relationship between infection with H. pylori and functional dyspepsia.
Psychological and social (psychosocial) factors - People with functional dyspepsia may be more likely to have certain mood problems, such as anxiety or depression. This is not to say that a person's pain is "in their head" or "made up", although treating the underlying depression or anxiety may improve a person's symptoms of abdominal discomfort.
Diagnosis
There are a number of reasons why a person can develop symptoms of dyspepsia. Organic (non-functional) dyspepsia can cause symptoms that are similar to those of functional dyspepsia, or the symptoms may be slightly different.
 |
| Pic courtesy getty images |
A doctor will perform a medical history and physical examination to narrow the possible list of causes, with special attention to the following: Is the pain "gnawing" or worsened by hunger? Is the pain worsened by certain movements or pressure on certain areas of the abdomen?
Do you take medications for pain, such as aspirin, ibuprofen? Do you have a history of ulcers? Do you have heartburn in addition to upper abdominal discomfort? Do you have intense pain in the upper right or middle of the abdomen?
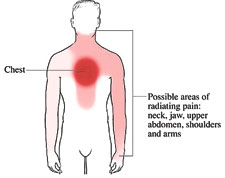
Does the pain extend to the back or between the shoulder blades? Does this happen periodically, along with vomiting, sweating, or feeling restless? Have there been changes in your bowel habits (eg, constipation or diarrhoea)? Have you recently unintentionally lost weight, vomited repeatedly, or had difficulty swallowing?
Testing recommendations
The best way to diagnose functional dyspepsia is not clear. People who are older than 45 or with serious symptoms, such as repeated vomiting, weight loss, difficulty swallowing, or a low blood count, should have an upper endoscopy procedure. People who are younger than 45 and who do not have serious symptoms are generally offered noninvasive tests. If symptoms fail to improve within four to eight weeks or if more serious symptoms develop, further testing, including upper endoscopy, is usually recommended. Other diagnostic tests may be recommended in selected cases.
Treatment
Understanding the condition - Being diagnosed with functional dyspepsia may be a relief to some people and a frustration to others. It is important to understand that symptoms are not imaginary. One or more treatments may be recommended, often in combination; having realistic expectations of the benefits of treatment may help to reduce frustration. If there are mood problems, such as anxiety or depression, an evaluation with a mental health specialist (eg, psychologist, counsellor) may be recommended.
Lifestyle changes - Some people benefit from avoiding fatty foods (which can slow the emptying of the stomach), and eating small frequent meals. Foods that aggravate symptoms should be avoided, if possible, although eliminating entire food groups is not recommended. If there are questions about which foods should be avoided, this should be discussed with a doctor and/or dietician.
Medications - Certain medications may help to reduce the symptoms of functional dyspepsia.
H. pylori therapy - Treatment of H. pylori is recommended if an ulcer is diagnosed.
Acid reducing medications - Some people benefit from treatment with medications that inhibit or reduce the production of stomach acid (eg, H2 blockers and proton pump inhibitors).
Visceral analgesics - As mentioned previously, some people with dyspepsia are sensitive to enlargement (distension) of the stomach. Medications that relieve visceral pain are being studied.
Pain medications - Low doses of an antidepressant medication may be recommended to reduce pain, even if the patient is not depressed. The doses of these drugs are typically much lower than that used for treating depression. It is believed that these drugs reduce pain perception when used in low doses. Their full effect may not be seen for weeks to months.
Dyspepsia is typically a relapsing condition. In studies, 60 to 90 percent of people continue to have symptoms of varying degrees two to three years after being diagnosed. However, most people feel better once their condition has been properly diagnosed, and many will respond to the treatments discussed above.
(The writer is Consultant Physician , Sri Lanka Police Hospital Colombo) |


