

![]()
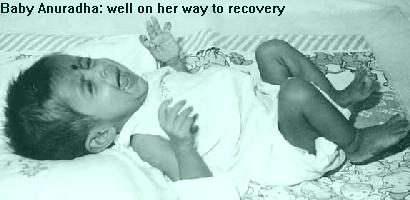
Anuradha had been in and out of hospital many times because of noisy and difficult breathing. She refused her feeds and was consequently losing weight. She was blue and moribund. Her parents from Kalutara, could not afford to take care of her and she was sent to the Cardiology Unit for further investigations.
At the Cardiology Unit, an echo cardiogram was done (investigations to reveal the structure and anatomy of the heart and blood vessels using sound waves). A diagnosis of complete congenital heart disease called Total Anomalous Pulmonary Venous Drainage (TAPVD) was made.
 This
condition occurs when , the oxygenated blood from both lungs drain into the
right side of the heart instead of the left side. This is abnormal and leads to
mixing of the blood in the heart. The blood reaches the left atrium through a
hole in the heart called the atrial septal defect. This also puts a heavy load
on the right side of the heart and some of this blood re-enters the lungs,
overloading them. This leads to an increase in the pressure in the lungs which
after a time becomes irreversible.
This
condition occurs when , the oxygenated blood from both lungs drain into the
right side of the heart instead of the left side. This is abnormal and leads to
mixing of the blood in the heart. The blood reaches the left atrium through a
hole in the heart called the atrial septal defect. This also puts a heavy load
on the right side of the heart and some of this blood re-enters the lungs,
overloading them. This leads to an increase in the pressure in the lungs which
after a time becomes irreversible.
The National Hospital Cardiac Unit operates on both adult and paediatric heart patients. The type of operations done are valve repairs and replacements, coronary artery bypass surgery, correction of congenital heart defects like VSD ( ventricular septal defects) Fallots tetralogy etc. Sri Jayewardenepura Hospital is the only other hospital in the country to have such a unit in the state sector.
Baby Anuradha was a genuine cardiac emergency. A few blood tests were done to check the condition of the baby. Chest x’rays were done. Antibiotics were also given in addition to the anti-heart failure drugs. Consultant Anaesthetists Dr. Mrs. Hemantha Perera and Dr. Mrs. Kumudini Ranatunga prepared the baby for the operation.
The surgery was performed in operating theatre C, which is the only one equipped for open heart surgery in the hospital.
The baby was taken in at 8.30 am and aneasthesia was induced. A tube was passed into the trachea and connected to a paediatric ventilator. Several lines were introduced into the blood vessels to administer drugs and to monitor the baby’s pressure continuosly during and after surgery.
The chest was opened by cutting the sternum with a saw. Two small tubes were introduced into the aorta and the right atrium, and the heart was connected to a heart-lung machine. Now the baby’s circulation was maintained by this machine. The temperature of the baby was reduced to 16 dg. C by cooling the blood. Then the circulation was stopped completely and the chamber of the heart was opened.
 The
defect was visualised and assessed using a piece of pericardium from the baby’s
body. By using sutures the defect was corrected. All this took 25 minutes. Then
the circulation was restarted and the baby rewarmed to 37 dg. C. The
ventilation was restarted and the baby was disconnected from the heart-lung
machine and the heart was gradually allowed to take over the circulation.
When the infant patient achieved stability the chest was sutured back and the
baby transferred to the intensive care unit.
The
defect was visualised and assessed using a piece of pericardium from the baby’s
body. By using sutures the defect was corrected. All this took 25 minutes. Then
the circulation was restarted and the baby rewarmed to 37 dg. C. The
ventilation was restarted and the baby was disconnected from the heart-lung
machine and the heart was gradually allowed to take over the circulation.
When the infant patient achieved stability the chest was sutured back and the
baby transferred to the intensive care unit.
The baby was connected to the monitor and ventilator and closely observed for the next few days. Drugs were administered through infusions using special syringe pumps to administer minute doses. After three days the baby was weaned from the ventilator. A week later she was transferred to the cardiac ward. She is now feeding well and gaining weight. She has no shortness of breath and is alert and full of smiles.
Continue to Plus page 10 -Europa: is it high life or primordial sludge?
Return to the Plus contents page
![]()
| HOME PAGE | FRONT PAGE | EDITORIAL/OPINION | NEWS / COMMENT | BUSINESS
Please send your comments and suggestions on this web site to
info@suntimes.is.lk or to
webmaster@infolabs.is.lk